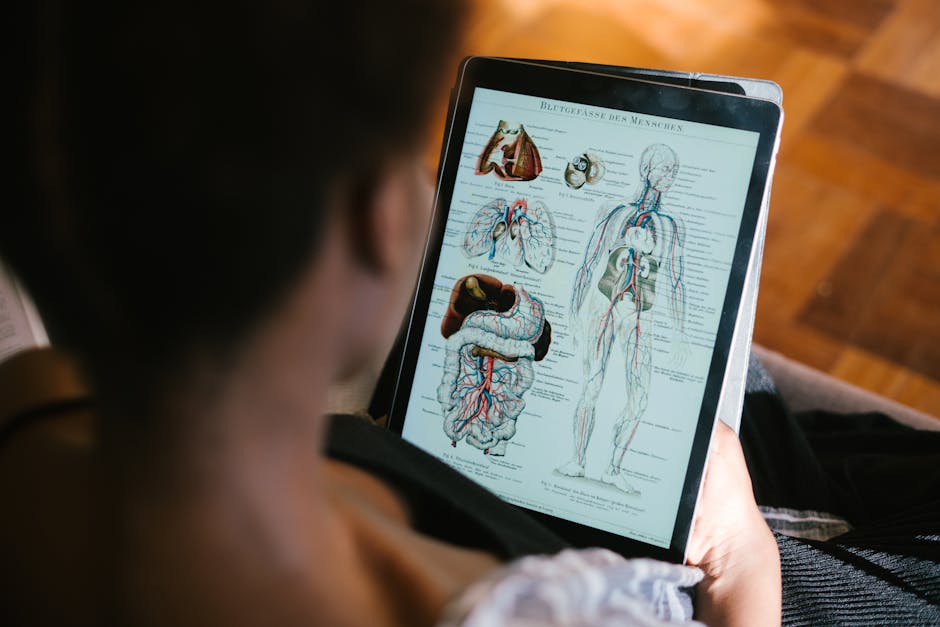
- Cancer almost never spreads to the heart despite its rich blood supply.
- Metastasis to the heart is extremely rare, occurring in only 0.005% of cases.
- The heart’s environment is inhospitable to cancer colonization due to high oxygen levels and constant mechanical motion.
- Research suggests the heart’s unique metabolic profile may disrupt cancer cell survival and adhesion.
- Understanding the heart’s resistance to metastasis could lead to new strategies to block cancer’s spread elsewhere in the body.
Why does cancer almost never spread to the heart? Despite being a vital organ with a rich blood supply—prime real estate for circulating tumor cells—metastasis to the heart is extraordinarily rare. This paradox has puzzled oncologists and biologists for decades. While cancers commonly spread to the lungs, liver, brain, and bones, the heart remains a near-forbidden zone. What biological defenses could be so effective? And could understanding them unlock new strategies to block cancer’s spread elsewhere in the body? These questions have gained renewed urgency as researchers uncover surprising clues hidden in the heart’s unique physiology.
The Heart’s Unusual Resistance to Metastasis
Metastatic cancer occurs when tumor cells break away from their primary site, travel through the bloodstream or lymphatic system, and form new tumors in distant organs. Given that the heart pumps about 5 liters of blood per minute—carrying with it any rogue cancer cells—it would seem like an inevitable target. Yet, autopsy studies show that only about 0.005% of metastatic cancers involve the heart. This resistance isn’t due to lack of exposure; tumor cells pass through the heart constantly. Instead, research now suggests the heart’s environment is fundamentally inhospitable to cancer colonization. Unlike other organs, it combines high oxygen levels, constant mechanical motion, and a unique metabolic profile that may disrupt cancer cell survival and adhesion.
Biological and Mechanical Barriers in the Heart
Recent studies, including a 2023 analysis published in Nature, point to several interlocking defenses. First, the heart’s relentless contractions—over 100,000 times per day—create shear forces that may physically dislodge arriving cancer cells before they can anchor. Second, cardiomyocytes (heart muscle cells) consume energy at an extraordinary rate, primarily using fatty acids in a high-oxygen environment. This metabolic landscape may starve cancer cells, which typically rely on glycolysis (sugar fermentation) even in oxygen-rich settings—a phenomenon known as the Warburg effect. Additionally, the heart expresses high levels of immune-activating molecules, potentially enhancing local surveillance by T-cells and macrophages. Together, these factors may create a ‘hostile microenvironment’ that prevents tumor establishment.
Skeptical Views and Emerging Counter-Evidence
Not all researchers agree that the heart is inherently resistant. Some argue that reported cases of cardiac metastasis are underdiagnosed due to limited clinical monitoring and the organ’s low tolerance for biopsy. A 2022 review in ScienceDaily highlighted that up to 20% of terminal cancer patients may have undetected heart involvement at autopsy, suggesting the rarity might be overstated. Others note that primary heart cancers, though extremely rare (less than 0.1% of all heart tumors), do exist—raising questions about why the organ resists metastasis but not primary tumors. Furthermore, certain aggressive cancers, like melanoma and lung cancer, do metastasize to the heart more frequently than others, implying that tumor-specific traits may override organ defenses.
Real-World Implications for Cancer Treatment
Understanding the heart’s resistance could reshape cancer therapy. If scientists can isolate the mechanisms that repel metastatic cells, they might engineer synthetic environments or drugs that mimic these effects in vulnerable organs. For example, therapies that increase tissue stiffness or oxygenation—mimicking the heart’s mechanical and metabolic conditions—could deter tumor seeding in the liver or brain. Additionally, boosting local immune activity in high-risk areas might replicate the heart’s natural surveillance. Already, some labs are exploring nanoparticles that release fatty acids in tumor-prone tissues to disrupt cancer cell metabolism. These insights may also improve patient monitoring: if cardiac metastasis is truly rare, its presence could signal unusually aggressive disease, prompting earlier intervention.
What This Means For You
For patients and clinicians, the heart’s resistance offers a rare piece of hopeful biology in the fight against cancer. While not a cure, it highlights that the body already possesses natural defenses we can learn to harness. Future treatments may not only attack cancer directly but also strengthen the body’s innate ability to repel it. This shift—from targeting tumors to fortifying healthy tissues—could lead to more durable outcomes and fewer side effects.
Still, many questions remain. Do all cancer types respond equally to the heart’s defenses? Could aging or heart disease weaken this protection? And most importantly, can we replicate these protective mechanisms in other organs without harming their function? As research continues, the heart may prove to be not just a pump, but a blueprint for a new generation of cancer therapies.
Source: Zmescience