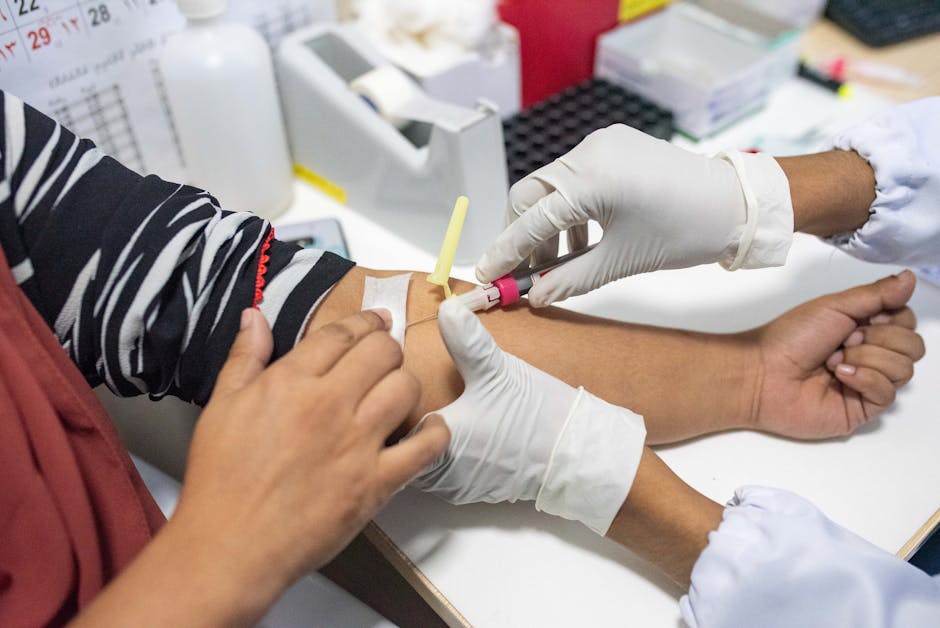
- Biotin supplements, popular among cancer patients for hair growth, may interfere with hormone and tumor marker tests.
- High-dose biotin may mask recurrence in cancer patients, leading to delayed or missed diagnoses.
- Cancer patients are at risk of taking excessive biotin from over-the-counter supplements, often unaware of its potential impact.
- Medical experts warn that biotin supplements may undermine accurate diagnostics, a critical tool in cancer monitoring.
- Cancer patients should consult their doctors before taking biotin supplements, as they may pose a risk to their care.
At a clinic in suburban Chicago, a 47-year-old breast cancer survivor sat anxiously in an exam room, awaiting her quarterly blood work results. She had completed chemotherapy six months earlier and was clinging to signs of normalcy—her hair had started to grow back, thanks, she believed, to daily biotin supplements. But when the oncologist walked in, his expression was unreadable. Her tumor markers were normal, but too normal. Suspiciously so. It wasn’t until he learned she’d been taking 10,000 micrograms of biotin daily—a common over-the-counter dose—that the pieces fell into place. The supplement, marketed as a beauty booster, had likely interfered with her hormone and tumor marker tests, potentially masking a recurrence. This moment, repeated across clinics nationwide, underscores a quiet but growing crisis: a vitamin touted for healthier hair may be undermining one of medicine’s most vital tools—accurate diagnostics.
Biotin’s Hidden Risk in Cancer Monitoring
Biotin, also known as vitamin B7, plays a role in metabolic function and is naturally found in foods like eggs, nuts, and salmon. However, in recent years, high-dose biotin supplements have surged in popularity, particularly among cancer patients grappling with hair loss after chemotherapy. Sold with bold claims of promoting thicker hair and stronger nails, these supplements are often perceived as harmless. But medical experts are now raising alarms. According to the U.S. Food and Drug Administration (FDA), biotin can interfere with immunoassays—blood tests that rely on biotin-streptavidin binding, a common method in clinical diagnostics. When biotin levels are elevated, test results for critical markers like thyroid hormones, troponin (a heart damage indicator), and cancer antigens such as CA-125 and PSA can appear falsely normal or abnormally low. This distortion may lead to missed diagnoses, delayed treatments, or inappropriate care decisions. A 2021 study published in The Journal of Applied Laboratory Medicine found that even standard over-the-counter doses can cause significant interference.
How We Got Here: From Beauty Trend to Medical Hazard
The rise of biotin as a household supplement began in the 2010s, fueled by social media influencers and wellness brands touting it as a miracle cure for thinning hair. Despite a lack of robust clinical evidence supporting these claims, sales skyrocketed. The global biotin market, valued at over $170 million in 2022, continues to grow. Meanwhile, the medical community was sounding early warnings. As early as 2017, the FDA issued a safety communication alerting labs and clinicians to the risk of biotin interference. Yet, the message has struggled to reach patients. Many oncologists report that fewer than half of their patients disclose supplement use during medical visits. Compounding the issue, biotin is often included in multivitamins and “hair, skin, and nails” blends, making it easy to ingest unknowingly. The disconnect between consumer perception and clinical reality has created a blind spot in cancer care, where a well-intentioned effort to reclaim appearance may inadvertently compromise survival.
The Patients and Physicians on the Frontlines
For patients, the decision to take biotin often stems from a deep desire to regain control after the trauma of cancer treatment. Hair loss, while temporary, can be psychologically devastating, affecting self-esteem and identity. Dr. Lena Torres, an oncologist at Massachusetts General Hospital, explains, “Patients want to feel like themselves again. They see advertisements, hear stories from friends, and assume, ‘What’s the harm?’ But we’re now seeing cases where biotin use delayed the detection of metastatic disease by months.” On the other side, physicians are grappling with how to communicate these risks without dismissing patients’ emotional needs. Some clinics have begun integrating integrative medicine specialists to guide supplement use, while others distribute educational pamphlets. Still, the burden often falls on already overworked oncology teams to screen for something that isn’t routinely tested: biotin levels in the blood.
Consequences for Diagnosis and Treatment Pathways
The implications of biotin interference extend beyond individual patients. When tumor markers are falsely suppressed, oncologists may wrongly conclude that a patient is in remission, potentially postponing imaging scans or follow-up biopsies. In emergency settings, interference with troponin tests could lead to missed heart attacks. For thyroid function, misdiagnosis can result in inappropriate hormone therapy, affecting energy, weight, and mood—already fragile areas for cancer survivors. Laboratories are adapting by implementing biotin removal protocols and alerting clinicians when interference is suspected, but these measures are not yet universal. Moreover, most patients stop taking biotin only after being explicitly told, and even then, the vitamin can remain in the system for up to 72 hours, requiring careful timing before critical tests.
The Bigger Picture
This issue reflects a broader challenge in modern medicine: the unregulated proliferation of dietary supplements and the gap between consumer belief and scientific evidence. Unlike prescription drugs, supplements are not required to prove efficacy or safety before reaching shelves. As a result, millions take substances with little oversight, often unaware of potential interactions. The biotin-cancer diagnostic crisis is not an isolated incident but a symptom of a system where wellness culture outpaces medical guidance. It underscores the urgent need for better labeling, clinician education, and public awareness campaigns that treat supplements not as benign additions but as pharmacologically active agents.
What comes next may depend on how swiftly the healthcare system responds. Some experts are calling for mandatory biotin disclosure on lab requisition forms and routine screening for high biotin levels in high-risk patients. Regulatory agencies may need to reconsider labeling requirements for supplements containing high-dose biotin. For now, the message to patients is clear: consult your oncologist before taking any supplement. The quest to restore hair should not come at the cost of health—or truth in diagnosis.
Source: ScienceDaily