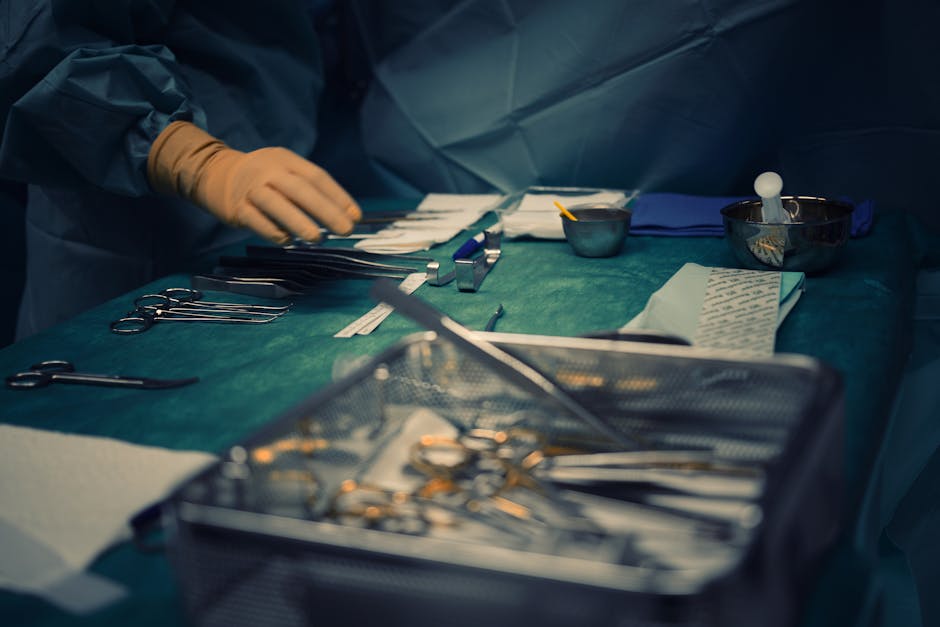
- Over 1 in 3 US hospitals now require healthcare workers to wear beard covers in certain areas, despite lack of clear evidence on their effectiveness.
- Beard covers are primarily enforced in interventional radiology suites, operating rooms, and sterile procedure areas, but not in other areas like medical offices.
- The Joint Commission’s accreditation standards drive the mandate for beard covers, but do not explicitly require them in all procedural areas.
- Some hospitals are interpreting these guidelines strictly, leading to new rules for full facial hair coverage, even in the absence of concrete scientific backing.
- The enforcement of beard covers has sparked debate among healthcare workers, with some questioning the evidence-based rationale behind these policies.
Why is a growing number of hospitals requiring healthcare workers to wear beard covers—despite no clear evidence they prevent infections? In interventional radiology suites, operating rooms, and sterile procedure areas, clinicians are now being told to shield facial hair with disposable fabric hoods, even as studies fail to show beards harbor more pathogens than clean-shaven skin. Some staff are shaving after decades of facial hair; others are pushing back, asking: is this evidence-based medicine or performance? With no mandates for covering eyebrows, eyelashes, or other natural hair, the focus on beards feels arbitrary to many frontline providers. Are these policies protecting patients—or just checking a bureaucratic box?
The Rise of Beard Covers in Sterile Settings
The mandate for beard covers in clinical environments, particularly in interventional radiology (IR) and surgical units, has surged in recent years—often driven by accreditation standards rather than peer-reviewed science. The Joint Commission, a major healthcare accreditation body in the U.S., requires that “facial hair must not interfere with the seal of respiratory protection devices” and recommends minimizing shedding of skin particles and hair in sterile fields. However, it does not explicitly mandate beard covers in all procedural areas. Hospitals, aiming to meet broad infection control benchmarks, have interpreted these guidelines stringently, leading to new rules requiring full facial hair coverage. Yet multiple studies, including a 2019 review published in Infection Control & Hospital Epidemiology, found no significant difference in surgical site infection rates between bearded and clean-shaven surgical teams. Despite this, the practice persists and is even expanding.
What the Evidence Says—And Doesn’t Say
Research into whether facial hair contributes to healthcare-associated infections (HAIs) has consistently failed to support the need for beard covers. A 2014 study in the Journal of Hospital Infection tested bacteria levels on the faces of bearded and clean-shaven men and found no meaningful difference. Another 2015 study of over 1,000 surgical procedures at a U.S. hospital concluded that surgeons with beards did not increase infection risk. The World Health Organization (WHO) does not recommend routine beard covering, instead emphasizing hand hygiene, proper sterilization, and appropriate use of masks and gowns. The absence of requirements for covering eyebrows or eyelashes—both sources of natural shedding—further undermines the rationale. Experts argue that if the goal is reducing particulate shedding, the focus should be on validated interventions like improved ventilation and stricter gowning protocols, not cosmetic changes to facial hair.
Counterarguments: Tradition, Perception, and Precaution
Some infection control officers and hospital administrators defend beard covers as a precautionary measure, arguing that while evidence is lacking, the potential risk justifies the policy. They cite the principle of “better safe than sorry,” particularly in high-risk environments like IR, where sterile fields are critical. Others emphasize appearance and patient perception: a clean, uniform look may boost confidence in the care team’s professionalism. There is also concern that facial hair might compromise the seal of N95 respirators, though this applies mainly to respiratory protection, not routine sterile procedures. Still, the inconsistency in enforcement—why beards but not mustaches, sideburns, or eyebrows?—reveals a policy driven more by tradition and visual conformity than microbial risk. As one hospital epidemiologist noted anonymously, “We’re managing optics as much as organisms.”
Real-World Impact on Healthcare Workers
The new rules are having tangible effects on clinicians’ personal and professional lives. Some physicians with long-standing beards are shaving for the first time in years, describing the change as a loss of identity or even a minor morale blow. Others report skin irritation from frequent shaving, raising new health concerns. In one Midwestern hospital, two IR technicians resigned over the policy, calling it “petty and unscientific.” Meanwhile, compliance efforts divert time and resources: hospitals purchase thousands of disposable beard nets annually, adding to waste and supply costs. Unionized nursing groups have begun challenging such mandates as workplace overreach, arguing that clinical policies should be grounded in data, not aesthetics. The broader concern is that when symbolic rules replace evidence-based ones, trust in institutional leadership erodes—and real infection risks may be overlooked.
What This Means For You
If you work in healthcare, especially in procedural or sterile environments, you may soon face similar mandates. Understanding the difference between evidence-based infection control and symbolic compliance is crucial. Ask for the data behind any new policy—especially those affecting personal appearance. Institutions should be transparent about whether rules stem from accreditation pressure, tradition, or peer-reviewed research. For patients, the takeaway is that not all hospital safety measures are equally effective; the presence of a beard cover doesn’t necessarily mean a safer environment. True infection prevention lies in proven practices: hand hygiene, sterilization, and teamwork.
As hospitals continue to adopt policies that look like safety but lack scientific backing, a critical question remains: how do we distinguish genuine patient protection from “infection theater”? And when ritual replaces rigor, who ultimately bears the cost—the staff, the system, or the patient?
Source: Reddit