- A recent Finnish trial found that arthroscopic partial meniscectomy may not provide meaningful benefits for patients with degenerative meniscal tears.
- The study, published in The New England Journal of Medicine, suggests that the procedure may even accelerate joint deterioration and increase the need for future interventions.
- Researchers randomly assigned 146 patients to receive either real or placebo surgery, with results showing no significant difference in pain relief or functional improvement.
- For years, millions of patients worldwide have undergone arthroscopic partial meniscectomy under the assumption it relieves pain and restores function.
- The results of the OPERA trial challenge the foundation of one of orthopedics’ most routine interventions, raising questions about the effectiveness of the procedure.
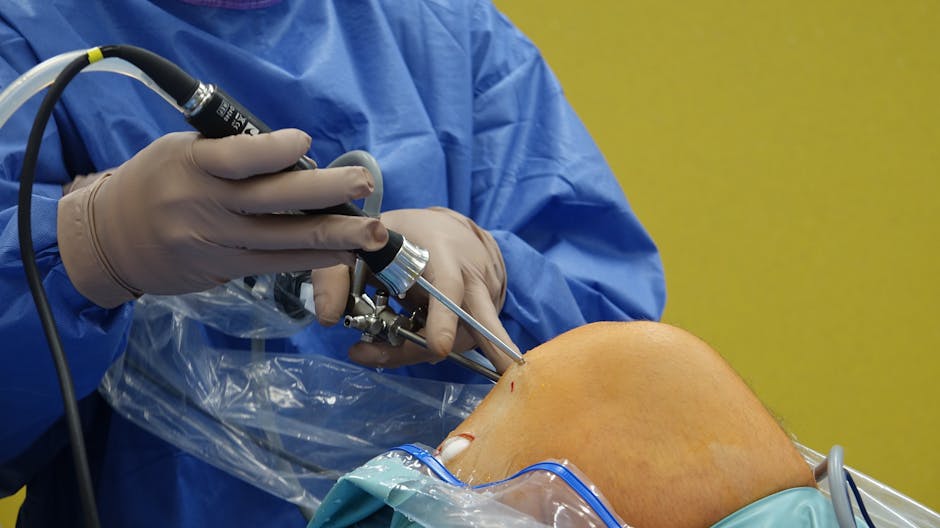
In a sterile operating room in Helsinki, a middle-aged patient lies under light sedation, legs draped in blue surgical cloth. The surgeon makes a small incision, inserts an arthroscope, and—unbeknownst to the patient—does nothing. No tissue is trimmed, no instrument touches the damaged meniscus. This is a placebo surgery, part of a rigorous, decade-long trial challenging the foundation of one of orthopedics’ most routine interventions. For years, millions of patients worldwide have undergone arthroscopic partial meniscectomy—a minimally invasive procedure to trim torn knee cartilage—under the assumption it relieves pain and restores function. But this carefully orchestrated sham operation, replicated across hundreds of patients, has helped produce a startling conclusion: the real surgery offers no meaningful benefit over the fake one. Worse, it may actually harm patients, accelerating joint deterioration and increasing the need for future interventions.
The Trial That Changed Everything
The Finnish OPERA trial, published in The New England Journal of Medicine after a full 10-year follow-up, tracked 146 patients with degenerative meniscal tears and mild to moderate osteoarthritis. Participants were randomly assigned to receive either arthroscopic partial meniscectomy or a placebo surgery involving diagnostic arthroscopy without intervention. Results showed no significant difference in pain relief or functional improvement between groups at any point during the decade-long study. In fact, patients who underwent the actual meniscectomy reported greater knee-related symptoms over time, including stiffness and instability. Imaging revealed faster progression of cartilage loss and osteoarthritis in the surgery group. Perhaps most concerning, 27% of those who had the real procedure eventually required total knee replacement, compared to 17% in the placebo arm—a 10-point difference that suggests the surgery may hasten joint decline. These findings echo earlier, shorter-term studies but now carry the weight of long-term evidence.
How We Got Here
Arthroscopic meniscectomy became a cornerstone of orthopedic practice in the 1980s and 1990s, promoted as a quick, low-risk solution for knee pain. By the 2000s, it was among the most common surgeries worldwide, with over 500,000 performed annually in the U.S. alone. Its popularity was fueled by patient demand, physician familiarity, and the intuitive appeal of “cleaning up” damaged tissue. Yet skepticism arose early. A landmark 2002 study by Moseley et al. first showed that sham surgery produced similar outcomes to real arthroscopy for osteoarthritis, challenging the procedure’s validity. Subsequent trials questioned its efficacy for meniscal tears, particularly in older adults where tears often stem from degeneration rather than acute injury. Despite this, the surgery persisted, supported by clinical inertia, financial incentives, and a lack of long-term data. The OPERA trial now fills that gap, offering the most definitive evidence to date that the procedure not only fails to help but may actively harm the joint.
The Surgeons and Scientists Behind the Shift
Leading the OPERA trial was Dr. Raine Paatela, an orthopedic surgeon and researcher at Helsinki University Hospital, whose team designed the study with meticulous attention to ethical and methodological rigor. Their motivation was not to discredit surgery, but to protect patients from unnecessary harm. “We perform thousands of these procedures every year,” Paatela said in an interview with Reuters, “but if they don’t work—or worse, cause harm—we have a duty to stop.” Other researchers, like Dr. Jeffrey Katz at Brigham and Women’s Hospital, have long advocated for conservative management of meniscal tears, emphasizing physical therapy and activity modification. These voices have often faced resistance from surgeons invested in the status quo, but the growing body of evidence is shifting the tide. Medical societies, including the American Academy of Orthopaedic Surgeons, now advise against arthroscopy for degenerative meniscal tears, though practice patterns change slowly.
Consequences for Patients and Health Systems
The implications of these findings are profound. Millions of patients may have undergone a procedure that provided no benefit and potentially shortened the lifespan of their knee joints. For individuals, this means unnecessary exposure to surgical risks—such as infection, blood clots, and anesthesia complications—without payoff. For health systems, it represents a massive waste of resources: each meniscectomy costs thousands of dollars, and the downstream costs of accelerated osteoarthritis and knee replacements are even higher. In the U.S., where healthcare spending is already bloated, eliminating ineffective procedures could save billions. More importantly, the findings urge a paradigm shift: treating knee pain not as a mechanical problem requiring surgery, but as a complex condition best managed through non-invasive strategies. Physical therapy, weight management, and strength training may offer more sustainable relief than a scalpel.
The Bigger Picture
This study is part of a broader reckoning in medicine over the efficacy of common procedures. From spinal fusions to hysterectomies, many interventions once considered standard are now being scrutinized under rigorous scientific scrutiny. The knee surgery trial underscores a critical lesson: just because a procedure is widely accepted, minimally invasive, and intuitively logical doesn’t mean it works. Medicine must rely on evidence, not tradition. As Dr. Atul Gawande has argued, the culture of surgery often prioritizes action over restraint, even when doing nothing may be the better choice. The OPERA trial is a powerful reminder that in healthcare, less can be more.
What comes next is a transformation in how knee pain is treated. Clinicians must re-educate patients, insurers must revise coverage policies, and medical training must emphasize conservative care. The era of routine meniscectomy may be ending—not with a dramatic ban, but with a quiet accumulation of evidence that could ultimately spare millions from unnecessary pain and surgery.
Source: ScienceDaily