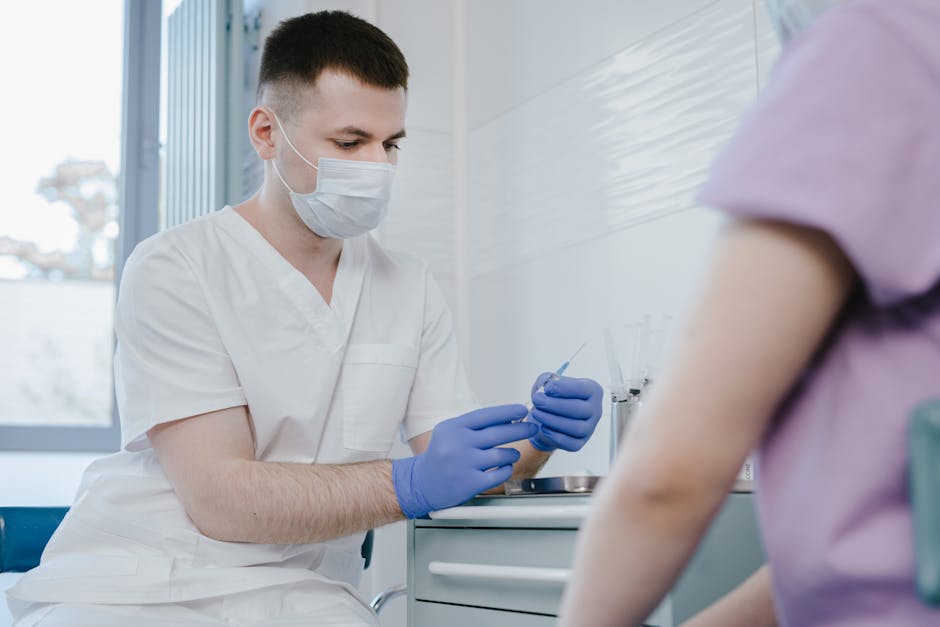
- The Big Catch-Up initiative, launched in 2023, aimed to vaccinate children who missed routine immunizations due to pandemic disruptions.
- Over 100 million vaccine doses were administered, reaching an estimated 18.3 million children across 36 high-need countries.
- The campaign targeted ‘zero-dose’ children, those who had never received a single dose of essential vaccines like measles and polio.
- While a significant achievement, millions of infants still remain unvaccinated annually, highlighting the ongoing challenge.
- Sustained investment in primary care systems is crucial for long-term success and to prevent future backsliding in vaccination rates.
How do you vaccinate millions of children who’ve never received a single dose? After years of pandemic-related disruptions to routine immunization programs, an estimated 25 million children worldwide—so-called “zero-dose” kids—were left vulnerable to preventable diseases like measles, diphtheria, and polio. In response, global health agencies launched the Big Catch-Up during World Immunization Week in 2023, aiming to reach 21 million under-immunized or unvaccinated children across dozens of countries. Now, with the initiative concluding in March 2026, data shows it delivered more than 100 million vaccine doses to an estimated 18.3 million children. While this marks a major milestone in global public health, experts warn that millions of infants still fall through the cracks each year—and without sustained investment in primary care systems, even the most ambitious campaigns may only offer temporary relief.
What Was the Big Catch-Up—and Did It Work?
The Big Catch-Up was a coordinated global immunization campaign led by the World Health Organization (WHO), UNICEF, Gavi the Vaccine Alliance, and national governments to reverse the backsliding of childhood vaccination rates during and after the COVID-19 pandemic. The initiative focused on 36 high-need countries across sub-Saharan Africa, South Asia, and parts of Latin America where disruptions had caused sharp declines in routine immunization coverage. By deploying mobile clinics, community health workers, and targeted outreach campaigns, the effort administered over 100 million doses of essential vaccines—including measles, polio, diphtheria-tetanus-pertussis (DTP), and pneumococcal conjugate vaccine—reaching approximately 18.3 million children. Of these, around 12.3 million were “zero-dose” children who had never been vaccinated before, and 15 million had specifically missed measles immunization. With the program on track to meet its 21-million-child target, health officials consider it a significant operational success in closing immunization gaps.
What Evidence Supports the Initiative’s Impact?
Data collected by WHO and UNICEF show that vaccination coverage in participating countries increased by an average of 18% for DTP3 (a key indicator of immunization program strength) between 2022 and 2025. In Nigeria, for example, mobile vaccination teams reached over 1.2 million previously unvaccinated children in rural and conflict-affected areas. In Pakistan, door-to-door campaigns helped boost measles immunization rates from 70% to 84% in targeted provinces. According to Dr. Soumya Swaminathan, former Chief Scientist at WHO, “The Big Catch-Up demonstrated that with adequate funding, coordination, and community engagement, we can rapidly scale up delivery even in fragile settings.” Independent monitoring by Gavi confirmed that 92% of supported districts reported improved cold chain infrastructure and data reporting systems. A 2025 WHO fact sheet also noted that measles cases declined by 31% in 2024 compared to pre-campaign levels, suggesting a direct public health benefit from the surge in immunization.
What Are the Counter-Perspectives and Limitations?
Despite its achievements, the Big Catch-Up has drawn criticism from some public health experts who argue that emergency campaigns cannot replace strong routine immunization systems. Dr. Samba Sow, Director of the Center for Vaccine Development in Mali, cautioned that “While mass campaigns are effective for catching up, they are expensive and unsustainable if not anchored in primary healthcare.” Others point out that the initiative did not fully address the root causes of vaccine inequity—such as underfunded health systems, vaccine hesitancy, and gender-based barriers to access. In some regions, cultural mistrust and misinformation led to resistance, particularly in areas where vaccines were delivered by external teams without long-term community integration. Additionally, humanitarian crises in countries like Sudan and Haiti limited access, leaving pockets of unvaccinated children untouched. There are also concerns about data accuracy, as some national reports may have double-counted children or relied on self-reported figures. As a result, while the 100 million doses are impressive, they may not fully reflect lasting immunity gains.
What Has Been the Real-World Impact So Far?
The most tangible outcomes of the Big Catch-Up are measured in lives saved and outbreaks averted. In Ethiopia, a surge in measles vaccination helped prevent what modeling predicted could have been a 40,000-case epidemic in 2024. In Afghanistan, where routine services remain weak due to political instability, the campaign provided a critical stopgap, vaccinating over 800,000 children against polio. Beyond immediate disease prevention, the initiative strengthened health systems by training over 50,000 community health workers and improving digital tracking tools in 22 countries. These gains may have long-term value, especially if integrated into national immunization programs. However, recent reports from BBC News indicate that in several countries, vaccination rates are already plateauing or declining again, suggesting that without continued support, progress could unravel quickly.
What This Means For You
For parents, policymakers, and global citizens, the Big Catch-Up offers a powerful example of what coordinated international action can achieve—but also underscores the fragility of public health gains. It confirms that even in the face of complex challenges, millions of children can be reached with life-saving vaccines when resources and political will align. However, the campaign’s success should not be mistaken for a permanent solution. Strengthening routine immunization systems, ensuring vaccine equity, and building trust at the community level remain urgent priorities. As new vaccines for malaria and respiratory syncytial virus (RSV) become available, the lessons from this initiative will be critical in ensuring they reach those who need them most.
Now that the Big Catch-Up has concluded, a pressing question remains: How can the world maintain this momentum without relying on emergency campaigns? With an estimated 13 million infants still under-vaccinated annually, the answer will require sustained funding, local ownership, and innovation in delivery systems. Can we build a future where no child is a “zero-dose” child—not through catch-up, but through consistent, equitable access?
Source: WHO